Revolution in Breast Cancer Prevention: AI System Detects Risk Up to Five Years in Advance
Key Takeaways:
•Newly Invented Artificial Intelligence Can Detect Breast Cancer Many Years before it surfaces
•The AI uses Deep Learning, Surveillance and Graphing to Uncover Breast Cancer at the earliest stage
•The AI’s Discriminatory power exceeds established models
A groundbreaking artificial intelligence system has been developed that can detect breast cancer up to five years before it fully develops, offering unprecedented potential for early diagnosis and prevention. This innovative AI model analyzes mammograms and other medical data, identifying subtle patterns that human doctors may miss, allowing for earlier intervention.
Breast cancer remains one of the most common and deadly cancers affecting women worldwide, claiming hundreds of thousands of lives annually. For decades, early detection has relied on mammograms read by radiologists, catching tumors once they are visible. But what if we could spot the warning signs years before a tumor fully develops? A groundbreaking artificial intelligence system has now made that possible, analyzing routine mammograms to predict a woman’s risk of developing breast cancer up to five years in advance.
AI Breast Cancer Detection and Diagnosis. Image: Breast Cancer Research Foundation
This isn’t science fiction—it’s here today. The AI works by utilizing deep learning algorithms to study vast datasets of medical images and patient histories, identifying early biomarkers and signs of cancerous changes. By detecting abnormalities long before they become clinically significant, this system could dramatically improve treatment outcomes, giving patients the opportunity to start therapies much earlier.
Tools like Clairity Breast, which received FDA de novo authorization in May 2025, and MIT’s Mirai model represent a seismic shift in oncology. By identifying subtle tissue patterns invisible to the human eye, these AI systems are transforming screening from reactive to truly predictive. The implications for survival rates, healthcare costs, and personalized medicine are profound.
How the AI Works: Seeing What Radiologists Can’t
Early detection has always been a key factor in increasing survival rates for breast cancer, and this new technology could become a game-changer in oncology. If widely adopted, it has the potential to reduce the number of advanced-stage diagnoses and the associated mortality rates. Furthermore, it could lead to more personalized treatment plans, as patients would be able to start treatment at a much earlier stage of the disease.
Traditional risk assessment tools, such as the Breast Cancer Surveillance Consortium (BCSC) model or Tyrer-Cuzick questionnaire, rely on factors like age, family history, breast density, and prior biopsies. These are helpful but limited, often missing women who appear low-risk on paper yet develop cancer.
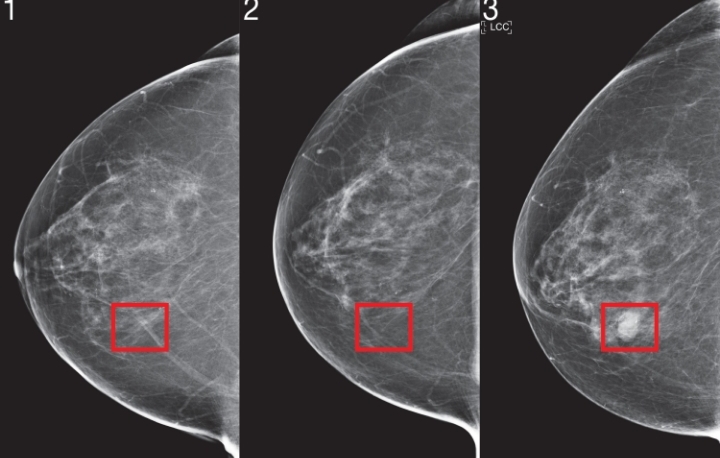
Robust artificial intelligence tools to predict future cancer. Image Source: MIT News Massachusetts Institute of Technology
The new AI systems flip the script. They use deep learning—a subset of artificial intelligence trained on massive datasets of mammograms paired with years of follow-up data. For instance, Clairity Breast was trained on millions of images linked to five-year outcomes. MIT’s Mirai model drew from over 60,000 mammograms and has since been validated on more than 1.9 million scans across 21 countries.
The AI doesn’t just look for obvious masses or calcifications. It analyzes micro-patterns in breast tissue: tiny changes in density, asymmetry between breasts, vascular patterns, and textural anomalies that signal future risk. In studies, AI scores were significantly higher in breasts that later developed cancer—even four to six years prior—compared to cancer-free ones. One analysis using a commercial AI (INSIGHT MMG) showed predictive power up to six years out, with scores doubling in at-risk tissue long before diagnosis.
Consider side-by-side mammograms from MIT research: an early scan might look “normal” to a doctor, but the AI flags a faint irregularity (highlighted in red). Years later, that same area reveals a tumor. Saliency maps—heatmaps generated by the AI—highlight exactly where the model sees risk, providing radiologists with explainable insights.
These models improve when fed multiple prior scans. One study found an AI using three years of mammograms was 2.3 times more accurate than standard clinical risk calculators. When combined with traditional models, accuracy skyrockets further.
The Evidence: Proven Accuracy and Real-World Validation
The science is robust. In a 2025 Radiology study, five AI systems outperformed the BCSC model in predicting five-year risk from normal mammograms of 13,600 women. Another Washington University study showed the AI identifying high-risk women 21 times more likely to develop cancer over five years than the lowest-risk group.
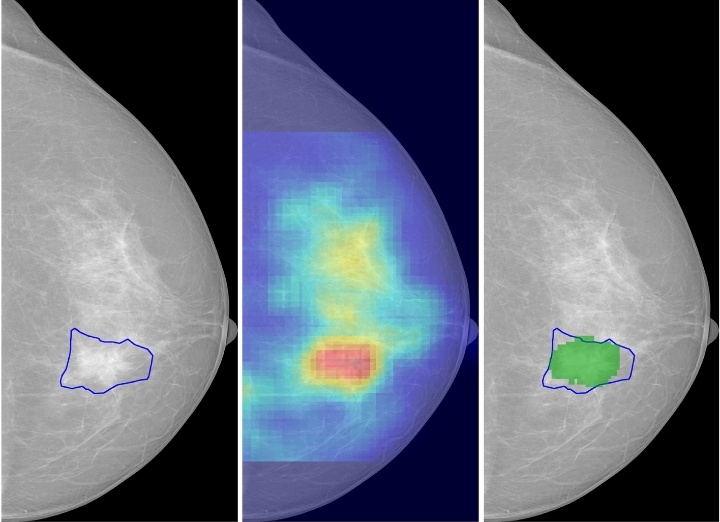
Saliency of breast lesions in breast cancer detection using artificial intelligence. Image Source – Scientific Reports
International validation adds credibility. Mirai performed consistently across diverse populations in Sweden, Taiwan, and beyond—crucial for global equity. A 2024 study in the Journal of the National Cancer Institute demonstrated AI could flag interval cancers (those appearing between screenings) up to 30% earlier, potentially reducing advanced diagnoses.
Even commercial tools not originally designed for long-term prediction, like Transpara, showed strong associations with invasive cancers 2–5.5 years later. The AI’s discriminatory power often matches or exceeds established models, and it’s particularly effective for dense breasts—a known challenge in mammography.
Life-Saving Benefits: From Screening to Precision Prevention
The potential impact is staggering. Breast cancer mortality drops dramatically with early intervention. By predicting risk five years out, clinicians can tailor screening: more frequent mammograms, supplemental MRI or ultrasound for high-risk women, or even preventive therapies like tamoxifen for those at elevated odds.
This could slash late-stage diagnoses, which account for much of the suffering and cost. Clairity’s developers emphasize seamless integration into existing workflows—radiologists get a validated five-year risk score alongside the standard report. No extra scans needed.
Broader benefits include reduced healthcare burden. Fewer unnecessary biopsies for false alarms. Cost savings from preventing advanced disease. And equity: AI can help close gaps in underserved communities where access to genetic testing or specialists is limited.
For patients, it’s empowering. A “normal” mammogram no longer means “no worry for years.” High-risk women gain time to act—lifestyle changes, closer monitoring, or genetic counseling—potentially averting cancer altogether.
Challenges and Ethical Considerations
No technology is flawless. AI models require diverse training data to avoid bias; early systems sometimes underperformed in non-White populations or dense breasts common in younger or certain ethnic groups. Developers are addressing this through global datasets, but ongoing vigilance is essential.
Privacy concerns loom large with medical imaging data. False positives could cause anxiety and overtreatment, while false negatives might create false security. Regulatory oversight, like the FDA’s rigorous review for Clairity Breast, helps, but widespread adoption needs standardized guidelines and clinician training.
Cost and access matter too. While AI enhances existing mammograms, not every clinic has the infrastructure yet. In low-resource settings, this breakthrough could widen or narrow disparities depending on rollout.
Experts stress AI augments, not replaces, radiologists. Human oversight remains vital for nuanced cases.
The Road Ahead: A New Era of Predictive Oncology
This AI breakthrough is just the beginning. Researchers are expanding to other cancers, combining mammogram AI with genomics, blood biomarkers, and even wearable data for multimodal risk profiles. Imagine annual check-ups that forecast not just breast cancer but a personalized health roadmap.
With AI the landscape of breast cancer care is enormous. With continued development, this tool could become a standard in preventative healthcare, saving lives by detecting cancer in its earliest and most treatable form.
Clinical trials for Mirai and others are underway, with commercial launches like Clairity’s expected to accelerate adoption. By 2030, predictive AI could become standard in screening protocols worldwide.
Hope on the Horizon
The development of AI that detects breast cancer risk up to five years early marks a turning point in the fight against this disease. It shifts the narrative from “catch it early” to “prevent it from starting.” For the millions at risk, this means more time, more options, and more lives saved.
If you’re due for a mammogram, schedule it—your scan could now hold predictive power never imagined before. Talk to your doctor about emerging AI tools. Support research and equitable access to these innovations.
The future of breast cancer isn’t just brighter—it’s predictable. And with AI leading the way, prevention is no longer a dream but a data-driven reality. Together, we can turn early warnings into lasting victories.






Leave a Reply